Colorectal cancer is the second deadliest cancer in the United States when men and women are combined. Numerous studies have associated a person’s lifestyle to colon cancer, and death rates are 40% higher for African Americans than any other ethnic group.
Here’s more information about this disease and how to lower your risk.
The Stigma Behind the Disease
Colorectal cancer one of the most deadly of cancers, but it is one of the most preventable. However, the early detection lifesaving test, a colonoscopy, is invasive and often makes people very uncomfortable at the thought of one.
There is a stigma attached to the colonoscopy and the part of the body it’s associated with as well as what the procedure entails. Many people are embarrassed just saying the word “rectum”, but no one should ever die from embarrassment or fear of the procedure itself.
Late-Onset vs Early-Onset Colorectal Cancer
Men and women are equally at risk for colon cancer. Risk increases with age where 90% of cases are diagnosed in people 50 years old and older.
Young-Onset Colorectal Cancer: Recent research by the American Cancer Society is showing a 1% to 3% annual increase in colorectal cancer incidence in adults under age 50 (20- to 39-year-olds) while the incidence is declining in older adults.
According to the American Cancer Society study, people younger than 55 are 58% more likely to be diagnosed with late-stage cancer than older people. Cancer is typically not on the radar of young adults or their doctors, so symptoms are ignored (sometimes for years).
- Get screened regularly. Due to the increase in early-onset colorectal cancers, the American Cancer Society is recommending screenings start at age 45 instead of the long-standing recommendation of age 50. Your physician can decide which test is right for you (e.g., sigmoidoscopy, colonoscopy, CT scan, barium enema).
- Over 75% of colon and rectal cancer cases had NO risk factors, so regular screening is essential.
Why African-Americans Are at Greater Risk of Colon Cancer
African-Americans have the highest incidence and mortality rates of colorectal cancer of any ethnic group in the United States. Relatively little is known about the molecular mechanisms that associate more colorectal cancer deaths with African Americans than other ethnic groups, but here’s what we do know…
1. Researchers show that a higher percentage of African-Americans won’t schedule the test compared to other groups and are often diagnosed at a later stage of the disease. African-American men are especially likely to refuse a colonoscopy.
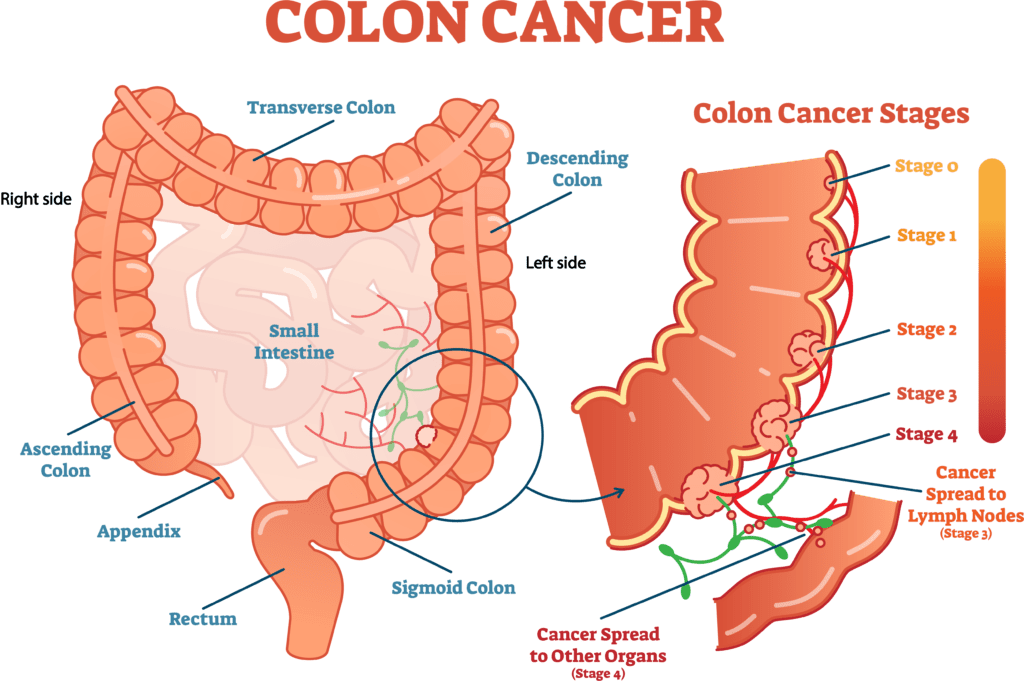
2. African-Americans are more likely to develop polyps deeper in the colon (on the right side) that a colonoscopy would reveal. The problem with the less invasive sigmoidoscopy exam (which uses a shorter tube, doesn’t need a full bowel prep like a colonoscopy) is that it only shows the left side of the colon).
According to the National Center for Health Statistics at the Centers for Disease Control and Prevention, the following groups will die from colorectal cancer:
- 1 in 41 black males
- 1 in 48 white males
- 1 in 44 black females
- 1 in 53 white females
3. African-Americans have other lifestyle factors:
- Higher tobacco-related illness
- More obesity
- Less physical activity
- Lower intake of plant-based foods that contain vitamins C and E (possibly tied to colon cancer)
Bile is to Blame
Bile is a fluid made and released by the liver and stored in the gallbladder until it is needed. Think of bile as your body’s ‘degreaser’. It assists with digestion by breaking down fats.
Bile acids stimulate the growth of bacteria, which convert the primary bile acids into secondary bile acids.
Bile acids, particularly secondary bile acids, have long been suspected as being cancer-causing. Eating more fat means more fat and bile acids in the colon.
Why Colon Cancer is Linked to Breast Cancer
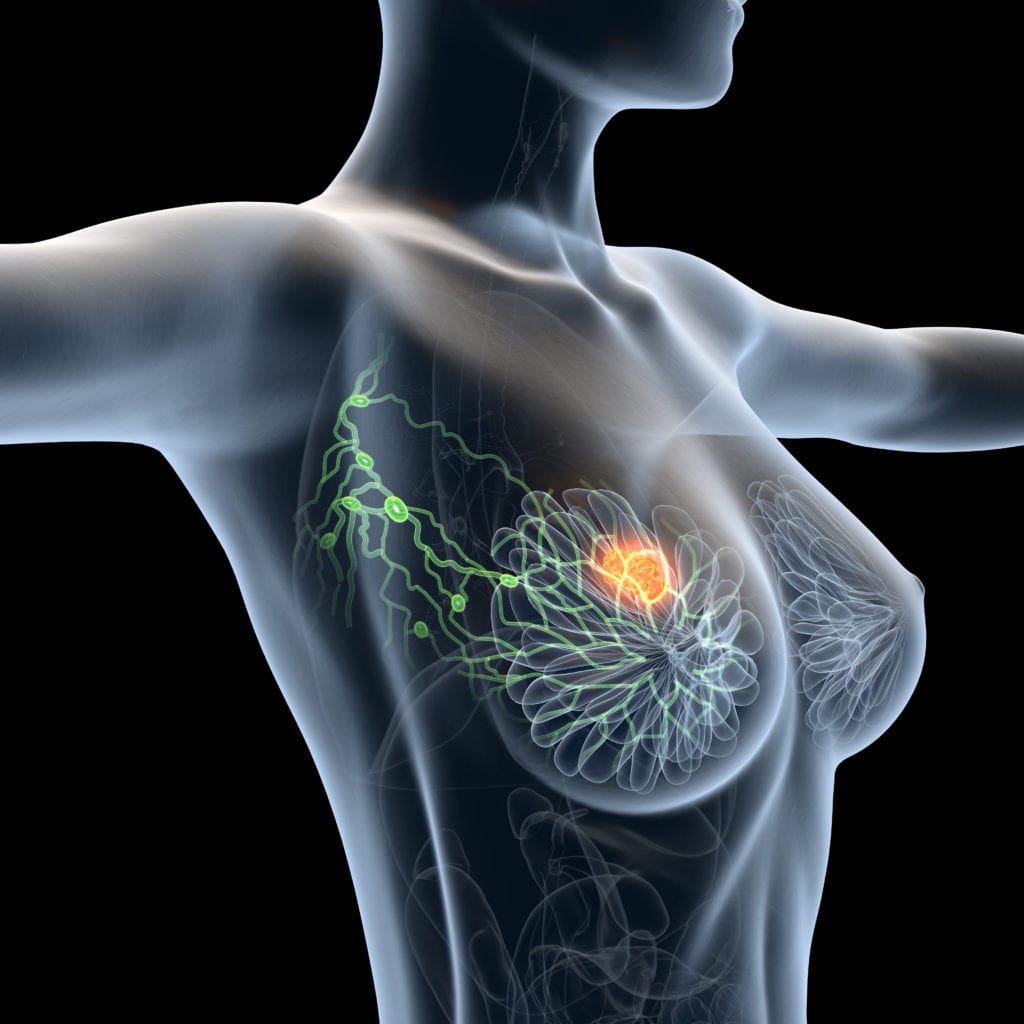 Bile circulates from the colon to the breast. Secondary bile acids can get absorbed into the bloodstream and travel throughout the body. This could also explain why a high saturated fat diet is also linked to breast cancer.
Bile circulates from the colon to the breast. Secondary bile acids can get absorbed into the bloodstream and travel throughout the body. This could also explain why a high saturated fat diet is also linked to breast cancer.
Meat vs Plant-Based Diet and Associated Cancer Risk
A study found that African Americans ate more protein (94 gm/day vs 58 gm/day) and more fat (114 gm/day vs 38 gm/day), meat, saturated fat, and cholesterol than Native Africans. Compared to African Americans, Native Americans produced a fraction of the secondary bile acids.
High Saturated Fats in the Diet
- A high intake of saturated fat is associated with high levels of bile, which is usually evident in colon cancer patients.
- High saturated fats + high levels of bile are factors that produce colorectal cancer tumors.
Bile Acids Increase Damaging Free Radicals
Increased bile acids increased production of free radicals. Free radicals damage DNA and the cells’ ability to repair themselves.
Immediate Dramatic Change After Switching to Plants
- After 12 days, subjects ate a diet rich in fat (50% fat) and meat and poor in dietary fiber. After one week they were switched to a low fat, fiber-rich diet. Hydroxyl radicals* dropped 13-fold.
*Hydroxyl radicals are one of the most destructive free radicals, which may increase colon cancer risk.
- After just one week on a plant-based diet, the growth of toxic and carcinogenic bacteria was reduced by 50%.
- After one month, their presence in the gut was reduced by 50%.
Family History
- Two to three times more likely to develop the disease in people with a parent, sibling, or child with colorectal cancer compared to those with no family history.
- Three to six times the risk of the general population when the relative was diagnosed at a young age or if there is more than one affected relative that of the general population.
- About 20% of all colorectal cancer patients have a close relative who was diagnosed with the disease.
Personal Medical History
- A personal or family history of inflammatory bowel disease, ulcerative colitis, or Crohn’s disease and cancers such as ovarian, breast, and endometrial may put you at higher risk for developing colon cancer.
Six Ways to Reduce Colon Cancer Risk Factors
1. Eliminate or limit animal fat. Limit meat to 3 oz. per week or less. Eat less butter, cheese, ice cream, baked goods.
2. Eat more plant-based foods. Emphasize plant sources, specifically whole grains, and plant proteins, such as nuts, beans, lentils, and tofu in addition to 3 servings of fruit, and 5+ servings of fruits and vegetables.
- Several studies suggest diet increases risk of both colon and rectal cancer (high consumption of red and/or processed meat and very low fruit and vegetable intake).
- It has long been known that people who follow a plant-based diet have less bile in their stools, so their capacity to form carcinogens in the colon is low. Plant eaters produce about 70% less of the secondary bile acids linked to cancer compared to meat eaters.
- Eat folate-rich foods, e.g., kale, Swiss chard, spinach, arugula, other dark green leafy vegetables. New study shows regular supplementation of 0.4 mg folic acid (B9) daily can reduce abnormal cell activity in the colon.


